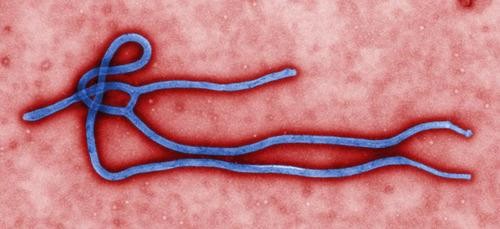
Photo by C.S Maureen
Yahoo News is reporting that two Americans infected with Ebola will be treated in the United States, marking the first time the deadly virus has been treated within U.S. borders.
The evacuations of Dr. Kent
Brantly and missionary Nancy Writebol are being facilitated by the State
Department and the Centers for Disease Control and Prevention. Emory
University in Atlanta announced at a press conference on Friday that it
will be treating two patients with the Ebola virus.
As of this week, Ebola virus disease (EVD) has killed more than 700 people,
according to the World Health Organization. There is no cure and no
vaccine for EVD, which kills between 60 and 90 percent of its victims.
The current outbreak — the largest in history — originated in Liberia
and has spread to neighboring countries, but it has been contained thus
far to West Africa.
The news that people infected with disease will be treated here in the U.S. sparked quite a reaction on social media, inspiring even a certain celebrity billionaire to take to Twitter in protest:
CDC director Thomas Frieden, M.D., called Ebola “a dreadful, merciless virus” on a press call on
Thursday, so it’s understandable that Americans would be concerned. But
the chance that someone in the general population will contract Ebola
is still extremely small.
"This is a very low-risk
situation for the general U.S. population," Diane Griffin, M.D.,
professor and chair in molecular microbiology and immunology at Johns
Hopkins University, told Yahoo Health. "Emory is a great place for [the
patient] to go. They are set up well to handle this type of situation."
Ebola is not spread like the cold
or the flu, she added. You could be sitting next to someone who is
infected and still not contract the virus. “It’s transmitted by very
close contact with people who are sick or with their bodily secretions,
such as blood, urine, and feces,” said Griffin. “It isn’t spread through
the air like most other viruses. It’s usually contracted by people who
are taking care of a sick person – either a health care worker in a
medical setting or by someone taking care of a sick family member at
home.”
Additionally, the infected
patient(s) will be treated in what sounds like the Fort Knox of
treatment centers. “Emory University Hospital has a specially built
isolation unit set up in collaboration with the CDC to treat patients
who are exposed to certain serious infectious diseases,” the hospital
said in a statement.
“It is physically separate from other patient areas and has unique
equipment and infrastructure that provide an extraordinarily high level
of clinical isolation. It is one of only four such facilities in the
country.”
The hospital says its staff is
well equipped to handle the incoming patients safely. “Emory University
Hospital physicians, nurses and staff are highly trained in the specific
and unique protocols and procedures necessary to treat and care for
this type of patient,” the statement continued. “For this specially
trained staff, these procedures are practiced on a regular basis
throughout the year so we are fully prepared for this type of
situation.”
Why Isn’t There an Ebola Vaccine?
According to a Newsweek piece
published on Friday, Brantley, the American doctor who was infected with
Ebola while treating patients in Liberia, received a blood transfusion this
week from a 14-year-old boy who recovered from the disease. Though this
procedure has been around for 20 years, its effectiveness against Ebola
remains largely unknown.
"This treatment has worked in
cases of other hemorrhagic fevers similar to Ebola, because the blood is
likely to have antibodies against virus," said Griffin. "There is good
data for other similar illnesses that shows you can treat people in this
way and improve their chances of recovery. I don’t know of any evidence
that it has worked for Ebola, but I’m sure they were pretty desperate,
so it’s certainly worth trying."
The National Institutes of Health announced on Thursday
that it will be begin human tests for an Ebola vaccine. Both the size
and the high-profile nature of the current outbreak have many people
wondering why it has taken this long. The main reasons, according to
Griffin, are that outbreaks are pretty infrequent and there hasn’t been
enough pressure globally to pursue a vaccine. “Even though the past
outbreaks in Africa have been tragic, they were quickly contained and
large numbers of people have not been at risk, she said. “Developing
vaccines is a very expensive process, and there just hasn’t been the
driving forces needed to move it beyond the animal testing phase.”
There are several experimental
vaccines that have been developed that work in animals, and a few of
them have been shown to work in monkeys, said Griffin. “It’s a tricky
situation,” she continued. “There is great reluctance to use an
experimental vaccine even in desperate times. Not all vaccines are safe,
and if it turns out the experimental vaccine does more harm than good,
it would be a public health disaster.”
No comments:
Post a Comment